What we talk about when we talk about community needs
The latest community health needs assessment by Rhode Island hospitals offers a good starting point for conversation
A few quick observations: patients who talk back and say no, for instance, when an occupational therapist attempted to put on a neck collar that was four sizes too small [for a medium female neck] are not rewarded for being outspoken [the painful experience was apparently not put into the medical records or shared with the surgeon].
The failure to share the results of blood tests conducted at the hospital with the skilled nursing facility resulted in the need to redo the blood tests, delaying recommended treatment for six days, extending my stay in rehab.
The success of the surgery as measured in the immediate end of chronic pain symptoms and stress caused by compression on the nerve, as well as the dramatic need for the surgery uncovered by the surgeon, stands in stark contrast to the difficulties of navigating the health care delivery system for three years, with one doctor refusing to order an MRI because I was deemed not a good candidate for surgery.
Translated, there is a need for patients’ voices to be heard and documented beyond being seen as a consumer of a commodity.
PROVIDENCE – For the third time in the last decade since the enactment of the Affordable Care Act, hospitals in Rhode Island have completed what is known as the 2019 Community Health Needs Assessment, creating a wealth of data regarding the analysis of community needs, looking at the populations served by each of the hospitals in Rhode Island.
In actuality, there were two community needs assessments conducted in Rhode Island – one by members of the Hospital Association of Rhode Island, taking a statewide collaborative approach, combining the findings of the seven hospital members, including Women & Infants Hospital, Butler Hospital, Kent Hospital [all part of Care New England], South County Health, Yale New Haven [Westerly Hospital], Landmark Medical Center, and CharterCARE Health Partnership. The work was conducted by the consultant Baker Tilly.
A separate Community Health Needs Assessment was conducted by Lifespan for its five member hospitals, including: Rhode Island Hospital, Hasbro Children’s Hospital, The Miriam Hospital, Newport Hospital and Bradley Hospital. [Lifespan is not a participating member of the Hospital Association of Rhode Island; its community health needs assessment has been posted on its website as of Sept. 30, as required by law.]
The importance of the findings is in the way that it creates a data snapshot at a time when Rhode Island is wrestling with the shape of the its future health care delivery system: the unresolved issues regarding efforts led by Gov. Gina Raimondo to create a unified academic medical center by the merger of Lifespan, Care New England and Brown University; the efforts being led by the Rhode Island Foundation to create a long-term statewide plan for health care delivery; and the ongoing initiative to develop Health Equity Zones by the R.I. Department of Health based on community health needs.
In addition, there are separate initiatives now underway: a community health needs assessment for the entire city of Pawtucket, led by Dr. Michael Fine in his new position as a health care liaison for the city; a collaboration between the School of Public Health and Blue Cross and Blue Shield of Rhode Island to create a survey analysis of how Rhode Island residents view their health, slated to be released later this month; and an ongoing effort by a compact of hospitals, health insurers, insurance regulators and physician group practices to analyze the drivers behind health care costs by looking at data from the All Payer Claims Database.
A deep dive
The process of the community health needs assessment conducted in collaborative fashion by the Hospital Association was informed by three key sources of data:
• Secondary data research, including statewide demographic, socioeconomic and health statistics, with a focus on the social determinants of health and unique health disparities, identifying community level strengths and opportunities.
• Community insight, including key informant surveys with community leaders, focus groups with health care consumers and partner meetings with Health Equity Zones and community partners.
• A focus on statewide priorities, including collective focus for collective impact, advanced population health management, and hospital and community-specfic strategies.
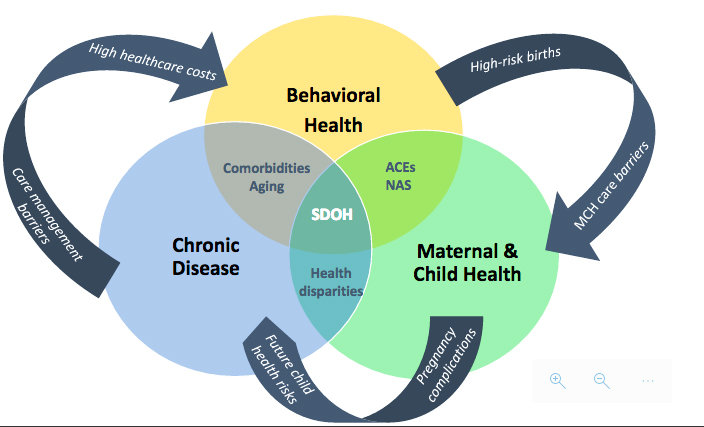
The top three areas of need identified by the collaborative community needs assessment conducted by the Hospital Association of Rhode Island member hospitals included: maternal and child health, behavioral health and chronic disease. [See first image above.]
Call it a shift in the paradigm of thinking about health care delivery, but the 2019 community health needs assessment conducted by the Hospital Association of Rhode Island emphasized the concept of “health equity” moving forward.
“Hospitals in Rhode Island are committed to ensuring health equity,” said HARI President Teresa Paiva Weed. She explained that the community needs assessment provided hospitals with the information they need to formulate and implement their strategic plans to ultimately work toward a healthier community.
Accordingly, each hospital has its own “implementation plan” to allocate specific resources and programs to address the priority needs for the 2019-2022 reporting cycle. In accordance with requirements of the Affordable Care Act, participating hospitals receive approval from their board of trustees for such implementation plans, with the final reports posted to each member hospital’s website.
Analysis of behavioral health needs
One of the top three community health needs identified was behavioral health, specifically with residents reporting poor mental health, with statewide totals for 2017 at 370.2 mental health provider rate per 100,000 population, compared to the national level of mental health provider rate of 2012.8 per 100,000 population. In addition, the analysis identified that the rate of drug-related deaths in Rhode Island was higher than the national average, but that outcomes were improving.
The areas of opportunity identified by the community needs assessment focused on youth and families, in order to break the cycle of trauma, with a specific focus on reducing neonatal abstinence syndrome to reduce the increases in child abuse and neglect and the increase in the number of children entering foster care due to substance use disorders.
Analysis of chronic disease needs
The focus on opportunities to improve the treatment of chronic disease in Rhode Island, based on the analysis of the community health needs assessment conducted by HARI, put the emphasis on addressing health and social disparities and the social determinants of health in core cities and priority populations, targeting co-morbidities among seniors and reducing e-cigarette and vaping use among teens.
The data showed that senior Medicare beneficiaries living in Rhode Island had higher rates of high blood pressure, high cholesterol, and depression than the national average, while diabetes, heart disease and Alzheimer’s disease matched the national averages.